
The uncertainties related to climate science present some unique challenges for policymakers and researchers alike. Drawing on lessons from the health care domain, where there are established mechanisms and processes in place for managing risk, Justine Lacey, Mark Howden and Chris Cvitanovic look at ways researchers can proactively support decision-makers. Could a similar ethics system to the one used by frontline medical professionals be implemented by climate scientists to enhance decision-making?
Given the significant and irreversible impacts of climate change on communities and the environment, there is increasing focus on how to best support decision-makers adapting to climate change. To date, much of this focus has been directed at assessing how decision-makers themselves navigate and manage risk and uncertainty in deciding to what extent they should adapt their own businesses and practices. We argue, however, that scientific researchers also have a key role to play in supporting these adaptation decisions.
Increasingly it is acknowledged that the communication of timely, useable and relevant research[Link will open in a new window] findings to those who will apply them is critical. However, it is equally important to identify and guard against the implicit risks that can be created in the communication of research findings. For example in the context of climate change, through researchers failing to outline the full list of adaptation options available to decision-makers, publicising their research findings as accepted and uncontroversial inputs into decision-making processes, or by not declaring other conflicts of interest. Such practices may be implicit or even exacerbated by our institutional structures[Link will open in a new window] but they have the potential to increase the risk exposure of decision-makers, with downstream impacts to broader societal well-being. However, such risks are rarely, if ever, examined in the context of adaptation decision-making.
What responsibilities do adaptation researchers have to decision-makers?
One way of increasing clarity about the existence and management of such risks is through distinguishing between the research and operational aspects of adaptation research, and how this interface is (or should be) disclosed. There is good reason to examine not only the uncertainties related to climate science itself, but also for researchers to be transparent and accountable for what kind of science is being undertaken and whether it is suitable for operational decision-making, how and by whom it is funded, and how it is communicated to decision-makers. Clarifying the distinction between the research and operational aspects of adaptation research can help to manage potential and unintended risks to adaptation decision-makers and provide clear guidance on ethical adaptation research. We believe a useful analogy can be drawn with the communication and implementation of findings in the health care domain where this distinction has been made operational.
Translating research to operational practice: Insights from the medical profession
The medical analogy is useful for three reasons. First, both the adaptation and health care domains have significant and direct impact on lives (or livelihoods). Second, there are significant challenges associated with translating basic research into improved outcomes for end users in both domains. Third, observing how frontline medical practitioners operate in order to protect the interests of their patients can offer insights into the translation and delivery of adaptation research that similarly protects the interests of the decision-maker over those of the researcher. In many ways, this also provides a pathway to ethical adaptation practice where such risks are actively acknowledged and managed.
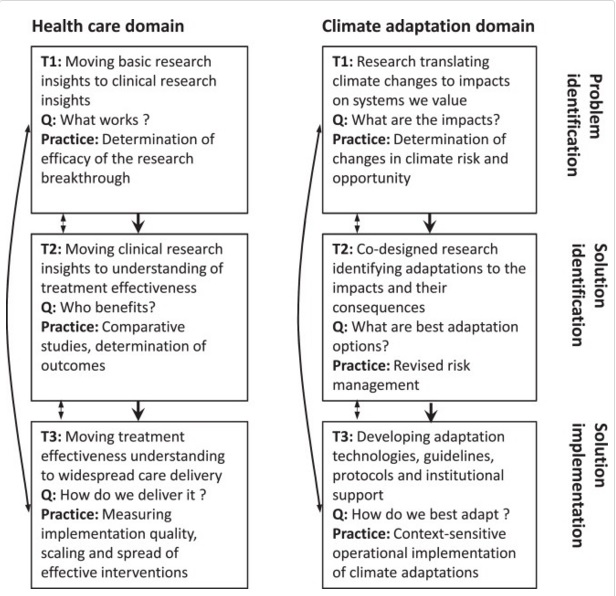
Drawing on established research translation activities in the health care domain, it is possible to conceptualise how adaptation research might similarly be understood as a series of distinct research activities (see Figure 1). For example, by conceptualising these transitions from basic research about the nature of climate impacts (T1) through to determining the best adaptation options (T2) and finally, the implementation of adaptation solutions (T3), we can draw out key differences in the roles and responsibilities of researchers at each stage, and also how risk to end-users can be managed. Risk occurs when research being generated at one stage is inappropriately applied in another. For example, research to identify effective adaptation solutions is critical but there also needs to be evidence to support the broad recommendation of those solutions to decision-makers so as not to unintentionally increase their risk exposure. This also means that the advice provided to decision-makers must be based on their personal contextual circumstances rather than who is providing the advice to them.
In the health care domain, there are established mechanisms and processes in place for managing differences of professional opinion which include established means of obtaining second opinions and processes for resolving any differences in the advice being provided. Patients are regarded as being in the position to make the final decision over their health care after they have had the opportunity to consider such diverse advice. Medical practitioners are required to constantly update their clinical knowledge to ensure they provide current advice, which means they are in a position to not only advise patients about how they might secure a second opinion or what the patient might need to consider in their circumstances but also to provide referral where a specialist medical practitioner is better equipped to provide patient care and advice. Similarly, the marketing of pharmaceuticals to health care professionals is monitored within a system of compliance and accountability in order to maintain the highest ethical standards in patient care and reduce the risks associated with financial inducements. These behaviours are governed by a recognised system of professional medical ethics developed primarily to protect the interests of patients.
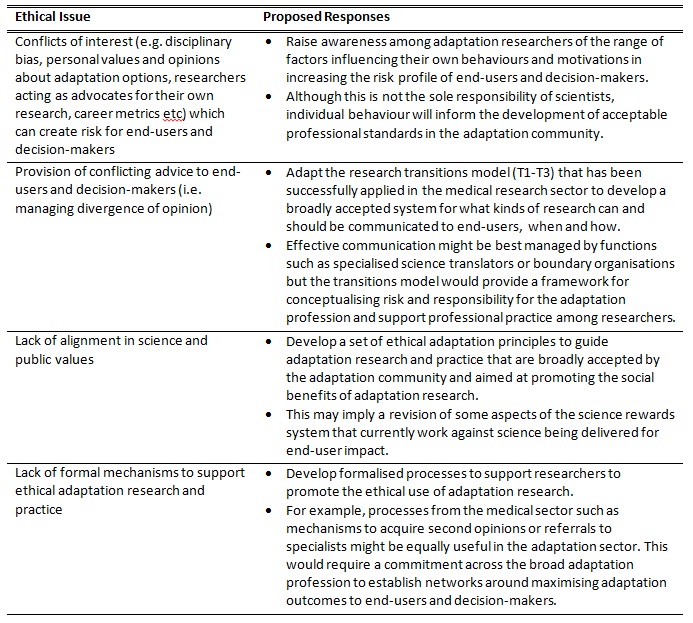
Could such a system of professional ethics be implemented among adaptation researchers with a view to enhancing the success of adaptation decision-making? Table 1 outlines some key ethical challenges facing adaptation researchers and a number of proposed responses.
Concluding remarks
In the adaptation domain, it is not yet clear if we have the appropriate checks and balances in place to support full disclosure in the communication of adaptation research findings to decision-makers (i.e. where both strengths and limitations of research and the costs and benefits of different adaptations are transparent). However, in recognising the ethical challenges that exist at the interface of adaptation research and decision-making, there are clear opportunities for researchers to more proactively manage the support of decision-makers.
Importantly, it must be recognised that ethical practice is not, in and of itself, error-free practice nor does it guarantee a certain outcome. Behaving in an ethical way does not inherently remove risk from adaptation research practice or decision making; rather it allows us to more explicitly manage certain types of risk related to the motivations and behaviours of those operating in this domain.
This article was originally published in the London School of Economics Impact Blog. Read the original article. This work is licensed under a Creative Commons Attribution 3.0 Unported License.
Note: This article gives the views of the authors, and not the position of the Impact of Social Science blog, nor of the London School of Economics.
About the Authors
Dr Justine Lacey is a senior social scientist with CSIRO Land & Water, specialising in the ethics of natural resource management in a number of contexts from water management through to minerals development in Australia and internationally. She is particularly interested in the ethical aspects of representing multiple and diverse interests in decision-making. Prior to joining CSIRO in 2011, she spent several years teaching and researching at Australian universities and five years working in the area of program monitoring and evaluation assessing the impact of a range of community development and natural resource management programs across Australia.
Dr Mark Howden is Chief Research Scientist with CSIRO Agriculture and Director of the Australian National University’s Climate Change Institute. He is recognised as a global expert on the impact of climate on food production and food security and how to adapt to those impacts. Mark has contributed to the United Nations Intergovernmental Panel on Climate Change (IPCC) via fifteen different roles across Working Groups since 1992, and holds the position of Distinguished Adaptation Scholar with the University of Arizona. He has published or contributed to more than 400 academic reports and books and has worked on greenhouse emissions mitigation and adaptation options for 28 years across a range of sectors. He has worked extensively with industry, communities and governments.
Dr Chris Cvitanovic is a social scientist with CSIRO Oceans and Atmosphere, where he works on identifying and overcoming the barriers to knowledge exchange among science and decision-making. Prior to joining CSIRO in 2013, Chris worked in the executive levels of the Australian Government Environment Portfolio where he delivered a range of policies and programs concerned with protecting Australia’s marine environment. Through this work, Chris developed a strong working knowledge of the barriers that prevent the integration of knowledge into decision-making processes, which led him to pursue his current research on the relationship between knowledge systems and adaptive governance.
