Malaysian outbreak
Cases of an unusual encephalitis were identified in pig farm workers in the Malaysian state of Perak in 1998, although, retrospectively, earlier human infections were diagnosed. These cases were initially diagnosed as Japanese encephalitis, a virus which causes neurological symptoms in humans and is endemic in Malaysia.

By late 1998, about 10 workers from a number of villages near Ipoh had also died. As a result, a Malaysian task force was formed to investigate. Through movement of infected pigs, the disease reached Sikamat, about 60 kilometres south of the Malaysian capital, Kuala Lumpur, in December 1998.
By March 1999, the disease spread to the major pig-producing area of Bukit Pelandok, in southern Malaysia, with many more human cases occurring. The outbreak resulted in 265 confirmed human cases with 105 fatalities.
Nipah virus is a paramyxovirus and is very closely related to Hendra virus. It was named after one of the Malaysian villages affected, Sungai Nipah, and was isolated by Dr Chua Kaw Bing from the University of Malaya in March 1999.
Tackling a new virus
As part of an International Task Force, Dr Peter Daniels and Dr John White from CSIRO's Australian Centre for Disease Preparedness (ACDP, then the Australian Animal Health Laboratory), travelled to Malaysia in March 1999 joining a US Center for Disease Control and Prevention (CDC) team.
Dr Daniels worked with the Malaysian Department of Veterinary Services, conducting animal post mortems and collecting animal samples for testing at ACDP in Geelong, Victoria, Australia.
Dr White worked with the Veterinary Research Institute in Ipoh to develop a test to show if animals had antibodies to the virus, indicating previous exposure.
The Malaysian Cabinet task force, together with international experts, developed a program of eradication. From 28 February 1999 to 26 April 1999, more than 900,000 pigs from affected areas were culled.
Preclinical research and development
There have been almost annual outbreaks of Nipah virus in Bangladesh since 2001, with neighbouring India reporting outbreaks in 2001, 2007, 2018 and 2019. With an average case fatality rate of 75 per cent according to the World Health Organization, and the total number of cases to date estimated to exceed 700, CSIRO has been at the forefront of global efforts to develop and evaluate countermeasures.
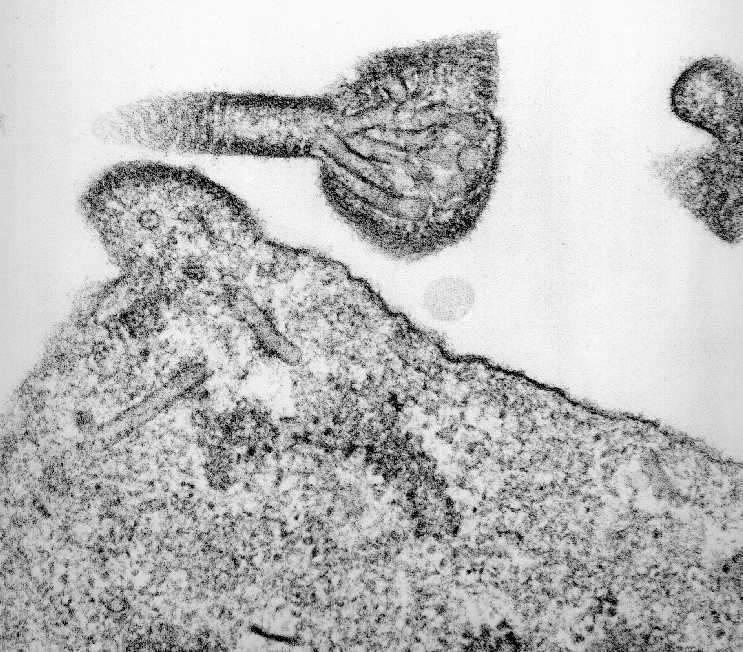
The CSIRO Dangerous Pathogens Team and colleauges at ACDP have undertaken transmission experiments with pigs to determine how the virus is shed from infected animals. They have used a range of techniques including electron microscopy, histology and genetic sequencing to research the virus.
This discovery accelerated research in many different areas, including the development of improved diagnostics, and vaccine candidates. In collaboration with US scientists, the group also evaluated a potential human vaccine to provide protection against both Nipah and Hendra viruses.
Research to understand more about zoonotic diseases is also being undertaken, with a focus on the interaction of bats and viruses and identifying and characterising new and emerging infectious agents.
Do you have preclinical research and development needs?
The CSIRO Dangerous Pathogens Team performs research, development and preclinical evaluation of medical countermeasures for dangerous pathogens affecting humans and animals (zoonoses), especially those requiring high containment at Bio-Safety Level-4 or 3.
Malaysian outbreak
Cases of an unusual encephalitis were identified in pig farm workers in the Malaysian state of Perak in 1998, although, retrospectively, earlier human infections were diagnosed. These cases were initially diagnosed as Japanese encephalitis, a virus which causes neurological symptoms in humans and is endemic in Malaysia.
By late 1998, about 10 workers from a number of villages near Ipoh had also died. As a result, a Malaysian task force was formed to investigate. Through movement of infected pigs, the disease reached Sikamat, about 60 kilometres south of the Malaysian capital, Kuala Lumpur, in December 1998.
By March 1999, the disease spread to the major pig-producing area of Bukit Pelandok, in southern Malaysia, with many more human cases occurring. The outbreak resulted in 265 confirmed human cases with 105 fatalities.
Nipah virus is a paramyxovirus and is very closely related to Hendra virus. It was named after one of the Malaysian villages affected, Sungai Nipah, and was isolated by Dr Chua Kaw Bing from the University of Malaya in March 1999.
Tackling a new virus
As part of an International Task Force, Dr Peter Daniels and Dr John White from CSIRO's Australian Centre for Disease Preparedness (ACDP, then the Australian Animal Health Laboratory), travelled to Malaysia in March 1999 joining a US Center for Disease Control and Prevention (CDC) team.
Dr Daniels worked with the Malaysian Department of Veterinary Services, conducting animal post mortems and collecting animal samples for testing at ACDP in Geelong, Victoria, Australia.
Dr White worked with the Veterinary Research Institute in Ipoh to develop a test to show if animals had antibodies to the virus, indicating previous exposure.
The Malaysian Cabinet task force, together with international experts, developed a program of eradication. From 28 February 1999 to 26 April 1999, more than 900,000 pigs from affected areas were culled.
Preclinical research and development
There have been almost annual outbreaks of Nipah virus in Bangladesh since 2001, with neighbouring India reporting outbreaks in 2001, 2007, 2018 and 2019. With an average case fatality rate of 75 per cent according to the World Health Organization, and the total number of cases to date estimated to exceed 700, CSIRO has been at the forefront of global efforts to develop and evaluate countermeasures.
The CSIRO Dangerous Pathogens Team and colleauges at ACDP have undertaken transmission experiments with pigs to determine how the virus is shed from infected animals. They have used a range of techniques including electron microscopy, histology and genetic sequencing to research the virus.
This discovery accelerated research in many different areas, including the development of improved diagnostics, and vaccine candidates. In collaboration with US scientists, the group also evaluated a potential human vaccine to provide protection against both Nipah and Hendra viruses.
Research to understand more about zoonotic diseases is also being undertaken, with a focus on the interaction of bats and viruses and identifying and characterising new and emerging infectious agents.
Do you have preclinical research and development needs?
The CSIRO Dangerous Pathogens Team performs research, development and preclinical evaluation of medical countermeasures for dangerous pathogens affecting humans and animals (zoonoses), especially those requiring high containment at Bio-Safety Level-4 or 3.
